What is physical health?
Physical health can be defined as the normal functioning of the body. Representing one dimension of total well-being, it's about how your body grows, feels and moves, how you care for it, and what you put into it.
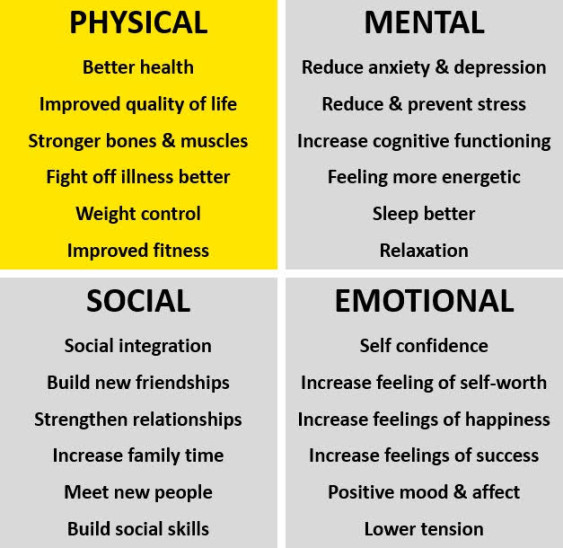
Pillars of Physical Health
Maintaining good physical health decreases your risk of developing conditions such as heart disease, stroke and some cancers. Being physically healthy also helps you to manage challenges by protecting you against fatigue, injury and illness.
Physical health is closely linked to mental health and an integral part of leading a healthy lifestyle. This is often taken for granted and it isn’t until we are sick, ill or injured that we put the time and energy in to looking after our physical health. It is important to regularly monitor your overall physical health and get a check-up if you (or someone you know) are concerned.
The four pillars of health are Sleep (and recovery), Nutrition, Physical Activity and Connection. The NZDF Health Hub provides everything you need to know about strengthening each of these pillars. Also check out the Staying on top of your game booklet.

|
|||

|

|

|

|
Sleep (and recovery)
Sleep is one of the most overlooked tools to enhance health and performance. Getting adequate sleep helps to prevent excess weight gain, heart disease and increased illness and disease. It is necessary to consider both the quantity and quality of your sleep and the try to maintain healthy sleep patterns.
After stressful activity, mental and physical, it is important to consider your needs for rest and recovery. Rest enables the body to repair itself to be fit and ready for the next activity. Recovery can be both passive (eg relaxing, sleeping) or active (eg a ‘recovery run’). For those who are training for a sporting or endurance event, it is important to consider the need for recovery both during training and in the lead-up. Whilst it is sometimes a useful tool to exercise when fatigued (particularly when training for endurance events), make sure that you are recovered enough to prevent injury. Training programmes should be dynamic to enable changes in response to injury or excess fatigue.
More information can be found in the Sleeping well section.
Nutrition
Adequate and appropriate nutrition helps support performance, recovery, mental clarity, and overall mood. This involves balancing meals with the necessary protein, carbohydrate and fat content, as well as ensuring required vitamin and nutrition intake.
Like a vehicle, the body performs best with the right fuel. If you put regular gasoline in a Formula 1 car, it will struggle to compete with the rest of the field and will likely end up making an early pitstop.
Good nutrition provides the body with the nutrients and fuel it needs to perform and recover. It also reduces stress and inflammation in the body, which is associated with injury, illness and mental health issues.
For detailed advice, see the Nutrition and supplements section. And check out this video explaining the surprisingly dramatic role of nutrition in mental health.
The surprisingly dramatic role of nutrition in mental health
00:00
Translator: Mayumi Oiwa-Bungard Reviewer: Queenie Lee
00:11
In 1847,
00:12
a physician by the name of Semmelweis
00:14
advised that all physicians wash their hands
00:17
before touching a pregnant woman,
00:18
in order to prevent childbed fever.
00:21
His research showed that you could reduce the mortality rates from septicemia,
00:26
from 18% down to 2%,
00:29
simply through washing your hands with chlorinated lime.
00:33
His medical colleagues refused to accept
00:36
that they themselves were responsible for spreading infection.
00:39
Semmelweis was ridiculed by his peers, dismissed,
00:43
and the criticism and backlash broke him down,
00:46
and he died in an asylum, two weeks later, from septicemia,
00:51
at the age of 47.
00:54
What I'm going to talk about today may sound as radical
00:57
as hand-washing sounded to a mid-19th century doctor,
01:00
and yet it is equally scientific.
01:03
It is the simple idea
01:04
that optimizing nutrition is a safe and viable way
01:08
to avoid, treat, or lessen mental illness.
01:13
Nutrition matters.
01:16
Poor nutrition is a significant and modifiable risk factor
01:20
for the development of mental illness.
01:23
According to the 2013 New Zealand Health Survey,
01:27
the rates of psychiatric illnesses in children
01:29
doubled over the last five years.
01:31
Internationally, there's been a 3-fold increase in ADHD,
01:35
a 20-fold increase in autism,
01:37
and a 40-fold increase in bipolar disorder in children.
01:42
And this graph here shows there's been a 4-fold increase
01:47
in the number of people who are on disability
01:50
as a direct consequence of an underlying psychiatric illness.
01:55
The rates of mental illness are on the rise.
01:59
So how are we dealing with this problem?
02:02
Currently, our healthcare system operates within a medical model.
02:07
Now, this means that you would typically be offered psychiatric medications first,
02:12
followed by psychological therapies,
02:15
and other forms of support.
02:19
Our reliance on medications as a front-line form of treatment
02:22
is evident from the increasing rates of prescriptions.
02:25
For example in 2012,
02:27
half a million New Zealanders - that's one-eighth of us -
02:31
had been prescribed an antidepressant;
02:33
that's 38% higher than five years previously.
02:37
Similarly, the rates of prescriptions for antipsychotics doubled,
02:41
from 2006 to 2011.
02:46
Given that this medical model
02:50
is fairly universal across all Western societies,
02:53
you would rightfully expect that it was working well.
02:57
And indeed, in some cases, these treatments save lives.
03:02
And I'm not here to dismiss it altogether.
03:05
However, if a treatment is truly effective,
03:09
then shouldn't the rates of disorder
03:12
and disability as a direct consequence of that illness
03:16
be decreasing rather than increasing?
03:19
That's why we need to consider the role that medications might be playing
03:23
in some of these outcomes.
03:25
If we take any class of medication: antipsychotics, anti-anxiety medications,
03:29
antidepressants;
03:31
the pattern is the same.
03:33
In the short-term,
03:34
these treatments are often very effective, but in the long-term, they aren't.
03:39
And in some cases, they're making life worse.
03:42
If we look at, for example, studies
03:46
that are being done on ADHD children treated with stimulants or Ritalin,
03:51
in the short-term,
03:53
they are better, and responding -
03:56
better responders than any other form of treatment,
04:00
but in the long-term,
04:01
they fare less well
04:05
than children who were never prescribed these medications.
04:08
Another study showed
04:09
that despite our ever-increasing reliance on antidepressants,
04:15
the recovery rates and relapse rates
04:17
are no better now than they were 50 years ago,
04:19
prior to the advent of these medications.
04:22
And children with depression
04:25
who were treated with antidepressants
04:28
are three times more likely to convert to bipolar disorder
04:31
than children who were never given these medications.
04:36
And people who were randomized
04:39
to stay on their dose of antipsychotic medications
04:43
are less likely to recover from schizophrenia in the long-term
04:48
than people who had been randomized
04:51
to a dose reduction or complete elimination of the drug.
04:55
And I can show you more and more studies
04:59
all highlighting the same bleak picture.
05:06
So,
05:08
pretty depressing.
05:10
(Laughter)
05:12
Is there another way forward?
05:16
Almost two decades ago,
05:17
my PhD supervisor at the time, Professor Bonnie Kaplan,
05:20
told me about some families
05:21
who were treating themselves with nutrients,
05:23
in Southern Alberta, Canada.
05:25
Now, they had bipolar disorder, psychosis, depression.
05:28
These are serious conditions, and my education in clinical psychology
05:32
had taught me that nutrition and diet were of trivial significance for mental health,
05:37
and that only drugs or psychotherapy could treat these serious conditions.
05:42
But she and others were publishing preliminary data
05:45
in the earlier part of this century,
05:47
showing people getting well and staying well.
05:50
And so, I decided to study the nutrients,
05:52
and that's what I've done for the last decade.
05:56
In 2009, I received some funding to run a randomized placebo-controlled trial,
06:01
using minerals and vitamins, also known collectively as micronutrients,
06:05
for the treatment of ADHD in adults.
06:09
And this study was published in the British Journal of Psychiatry
06:13
in April of this year,
06:14
and here's what we found.
06:16
Within just an 8-week period,
06:18
twice as many people responded in the micronutrient group
06:21
compared to placebo;
06:23
twice as many people went into remission in their depression,
06:26
in the micronutrient group.
06:27
Hyperactivity and impulsivity reduced into the normal, non-clinical range,
06:32
and those who were taking the micronutrients
06:34
were more likely to report
06:35
that their ADHD symptoms were less impairing and less interfering
06:40
in their work and social relationships
06:42
than people who were on the placebo.
06:44
And one year later,
06:46
those people who stayed on the micronutrients
06:48
maintained their changes or showed further improvement,
06:51
and those who switched to medications or stopped the micronutrients
06:57
actually showed worsening of their symptoms.
07:01
Now, I need to tell you something here,
07:03
and that is, when I say micronutrients,
07:05
I'm actually referring to a dose higher than what you'd get
07:08
out of a vitamin pill purchased on the supermarket.
07:12
In this study, we gave participants
07:14
up to 15 pills a day with 36 nutrients.
07:19
So it would be unlikely
07:20
that if you went and got an over-the-counter supplement,
07:23
you would unlikely see these positive benefits,
07:25
both because the dose is lower, and the breadth of nutrients is lower.
07:30
Now, these positive benefits are not confined to a single study.
07:36
My lab at the University of Canterbury
07:38
is the Mental Health and Nutrition Research Group,
07:40
and we've published over 20 papers in medical journals,
07:43
all documenting the benefits of micronutrients.
07:46
For example, this study here
07:48
showed that we could reduce the symptoms of bipolar disorder in children by 50%
07:53
with a simultaneous reduction of medications.
07:57
This study here
07:58
showed that we could reduce rates of probable posttraumatic stress disorder
08:06
from 65% down to 18%,
08:11
following the Christchurch earthquakes,
08:13
with a one-month intervention of micronutrients,
08:16
with no change in those not taking the nutrients.
08:19
Even one year later, those people who had received the nutrients
08:22
were doing better than those who didn't.
08:24
And we've just replicated these findings
08:26
in collaboration with researchers at the University of Calgary,
08:29
following the floods of June 2013, in Alberta, Canada.
08:34
To me, the message is clear,
08:35
that a well-nourished body and brain
08:38
is better able to withstand ongoing stress and recover from illness.
08:43
Giving micronutrients in appropriate doses
08:45
can be an effective and inexpensive public health intervention
08:50
to improve the mental health of a population
08:54
following an environmental catastrophe.
08:57
In my 20-year career, I have rarely seen
09:01
these dramatic responses from conventional treatments.
09:03
When people get well,
09:05
they get well across the board,
09:07
not only in the symptoms that we treated,
09:09
but also in other areas, like improved sleep,
09:12
stabilization of mood, reduction in anxiety,
09:15
and the reduction in need for cigarettes, cannabis, and alcohol.
09:18
My research and those around the world
09:21
have shown that 60 - 80% of people respond to micronutrients,
09:25
showing just how powerful this intervention is.
09:29
And internationally,
09:31
there have now been 20 randomized placebo-controlled trials -
09:34
this is the gold standard that we use to make clinical decisions -
09:38
showing that we can reduce aggression in prisoners,
09:41
slow cognitive decline in the elderly,
09:43
treat depression, anxiety, stress, autism, and ADHD.
09:51
And, they might even be more cost-effective
09:56
than current conventional treatments.
09:59
This study here documented the treatment of a 10-year-old boy with psychosis.
10:04
When his 6-month inpatient treatment with medications was unsuccessful,
10:09
he was treated with micronutrients.
10:12
Not only did the micronutrients
10:15
completely eliminate his hallucinations and delusions -
10:20
changes that were maintained six years later -
10:23
but the cost of the treatment was less than 2%
10:27
than the cost of the unsuccessful inpatient treatment.
10:31
The cost savings alone make it imperative
10:34
that our society pay attention to the wider benefits of this approach.
10:39
And there is more good news.
10:42
Treating -
10:44
Supplementing before mental illness emerges
10:47
can actually stop these problems from developing in the first place.
10:51
This fantastic study looked at 81 adolescents at risk for psychosis
10:57
and randomized them
10:58
to receive either Omega-3 fatty acids in the form of fish oils -
11:02
essential nutrients for brain health -
11:04
or placebo for a 12-week period.
11:07
One year later,
11:09
5% of those who received the fish oil had converted to psychosis
11:13
versus 28% of those on placebo.
11:16
That represents an 80% reduction
11:19
of the chances of you converting to psychosis,
11:23
simply through giving fish oils.
11:26
I wonder if I know what some of you are thinking.
11:30
I wonder if some of you are thinking,
11:31
"Hold on! Why don't I just eat better?"
11:36
"Why don't I just tell everyone to eat better?"
11:41
And indeed, there are some fantastic studies
11:45
that document the strong relationship between dietary patterns and mental health
11:50
although we're still in very early days of scientific investigation.
11:55
We don't know who would benefit from dietary manipulation alone,
12:01
and who may need the additional boost from extra nutrients.
12:06
But even in the last five years,
12:08
there have been 11 epidemiological studies,
12:11
cross-sectionally and longitudinally,
12:16
in large populations around the world,
12:19
all showing the same thing.
12:21
The more you eat a prudent or Mediterranean
12:25
or unprocessed type of diet,
12:27
the lower your risk for depression.
12:29
And the more you eat the Western diet or processed food,
12:33
the higher your risk for depression.
12:35
I know of only one study that has not found this association,
12:39
and not a single study shows
12:42
that the Western diet is good for our mental health.
12:47
(Laughter)
12:49
What is the Western diet?
12:51
Well, it's one that is heavily processed,
12:56
high in refined grains, sugary drinks, takeaways,
13:01
and low in fresh produce.
13:03
And the healthy diet is one that is fresh,
13:06
high in fruits and vegetables,
13:09
high in fish, nuts, healthy fats,
13:12
and low in processed foods.
13:14
What your grandmother would recognize as food.
13:17
(Laughter)
13:19
There are still many questions remaining
13:21
about the relationship between mental health and nutrition.
13:25
What role do genetics play
13:27
in determining who's going to respond to nutrients,
13:29
and who needs additional nutrients than what they can get out of their diet?
13:33
What role does an infected, inflamed gut play in the absorption of nutrients?
13:38
It's not we are what we eat;
13:39
it's we are what we absorb.
13:41
And what role do medications play
13:43
in determining how effective the nutrients are?
13:46
Combining medications and nutrients is actually complicated,
13:50
and we need more research in better understanding these interactions.
13:54
But ultimately, we need to know how long these good benefits last.
13:58
So with all of this data,
14:00
this rich data highlighting the power of nutrition,
14:03
I think we can make some individual and collective changes now.
14:08
We could reconsider our current treatment approach:
14:12
prioritize lifestyle factors,
14:15
healthy eating, exercise, supplements,
14:18
and when necessary, psychological treatments,
14:21
and save medications for when these approaches don't work.
14:26
If nutrients work,
14:27
then shouldn't they be covered through our healthcare system?
14:32
Take universal prevention seriously
14:35
by optimizing the nutrition of those who are vulnerable.
14:38
We don't wait for the heart attack to hit
14:40
in order for us to modify lifestyle behaviors
14:43
that we know contribute to heart disease.
14:45
It should be no different with mental health.
14:47
An easy way to implement universal prevention
14:50
would be to have pregnant women - not pregnant women:
14:54
midwives tell pregnant women about the importance of nutrition.
14:59
Nutrient-depleted mothers produce nutrient-depleted children.
15:04
Nutrient-poor foods during pregnancy
15:06
increase the chances that your child will have a mental health problem.
15:13
Learn about the risks of cheap, processed foods.
15:16
As Michael Pollan stated, cheap food is an illusion;
15:19
there is no such thing as cheap food.
15:22
The price is paid somewhere,
15:24
and if it's not paid at the cash register, then it's charged to the environment
15:29
and to the public purse in the form of subsidies,
15:31
and it's charged to your health.
15:34
All children need to learn how to cook.
15:36
All children need to know that food doesn't have to come in a packet.
15:40
Schools could reflect on the content of their lunch menus.
15:44
Children are too frequently rewarded with processed foods for good behavior.
15:50
We need to reflect on whether or not this pairing intuitively makes sense.
15:54
Ultimately, we have a responsibility to teach them
15:57
that every time they put something in their mouths,
15:59
they make a choice:
16:01
to eat something nourishing, or something nutritionally depleted.
16:05
In the 19th century, physicians were offended
16:09
when Semmelweis suggested they wash their hands before delivering babies.
16:13
We are now asking them to consider
16:15
whether the medications that they prescribed
16:18
are contributing to the poor long-term outcome
16:21
for some people with mental illness.
16:23
But eating well and when appropriate additional nutrients
16:28
can improve the mental health of many people.
16:32
I leave you with one last thought.
16:36
Randomized trials in the 1600s
16:39
showed that putting limes aboard ships headed out for long voyages
16:43
completely eliminated the 40% mortality from scurvy.
16:47
But it took 264 years for the British government
16:51
to mandate that all ships must carry citrus for their sailors.
16:55
How long will it take our society to pay attention to the research showing
17:01
that suboptimal nutrition is contributing to the epidemic of mental illness?
17:07
So this is my idea worth spreading:
17:09
Nutrition matters,
17:11
and if we're really ready to get serious about mental health,
17:15
we need to get serious about the critical role played by nutrition.
17:20
Thank you.
17:21
(Applause) (Cheering)
Physical Activity
The body is designed to move. Lack of exercise decreases range of motion within the body's joints causing pain and dysfunction. It also contributes to a decline in physical, mental and physiological health. Sedentary behaviours can lead to a variety of health consequences including weight gain, type two diabetes, cardiovascular disease and mood disorders.
On the flip side, too much exercise and stress can have an adverse effect, making the body susceptible to burnout and a compromised immune system. The body functions best with moderate amounts of work, stress and activity, coupled with rest to allow the body to repair and build stronger.

The beneficial effects of exercise on the brain
MAJ Jacques Rousseau on the type and timing of exercise to improve cognitive function.
good morning
0:13
hi everyone sorry for the late start uh we've had some technical difficulties getting the zoom meeting going uh but we should be good to go now
0:23
cool awesome right um what about the delay you know technology is a wonderful but it works
0:29
when it doesn't splits but we're all ready to go now um so I'm here today to give a little
0:36
bit of a talk on exercise and the Brain we know a lot about exercise in the body
0:41
I mean that that's been done over and over and over again you know
0:47
the body then exercise all the benefits that exercise has on our bodies but not
0:52
much is really known about how exercise affects the brain and it's sort of a new
0:57
area of research and science that's developing rather fast
1:02
um and what exercise does to the brain is quite amazing and if you exercise
1:09
program you're participating a bit of exercise you'll get really really good benefits from the exercise so I'm going
1:15
to talk to you a little bit about what you can do and how to supports your brain first of all I want you to think of a
1:24
couple of places in the world and think that you can get a link between them so the one is
1:30
ikara in Greece another is Okinawa in Japan and we've got Sardinia in Italy
1:38
a in Costa Rica what do you think
1:43
is the commonality between those places
1:49
yes that's a longevity so residents of those towns live the
1:56
longest and a lot of scientists have gone along and done a lot of research around why is this the case and they
2:05
found that physical activity is a way of life in these Villages or towns
2:11
so a lot of them went in hello okay in physical activity is a way of life how
2:16
does this impact on health and well-being and they've found that in these Villages uh dementia and
2:24
cognitive decline are the lowest approximately 75 percent less
2:31
in the western world okay so this is the the kinds of
2:37
researchers that we've done around us and there was a connection they've made is that physical activity
2:43
and it's mainly aerobic in the state but there's a lot of work going around uh uh
2:49
with strength training in the brain so they found that Earth activity and it's this stage we're looking a lot around
2:55
the aerobic activity that has really really good
3:01
benefits for the brain so
3:07
let's begin
3:14
what did I say about technology
3:20
so exercise we now know has profound impact on the
3:26
brain and this leads to numerous cognitive and mental health benefits and
3:32
what I'm going to do now I'm just going to go over some of these very briefly
3:39
with you so you just get an idea of what happens to this cognitive function and how the exercise depicts the brain
3:46
so if we have a look um when we exercise
3:51
this promotes better blood circulation and increases blood flow and and spot
3:58
that's a rich oxygenated blood that gets increased to the brain and this then
4:04
provides the brain with a lot of necessary nutrients of oxygen and this then helps improve brain function I mean
4:11
if you've got a lot of more nutrients a lot of oxygen going it's kind of like a no-brainer the brains kind of function better
4:19
then exercise has shown to improve production and release of various
4:26
neurotransmitters in the brain this includes endorphins um dopamine serotonin and nor
4:34
epinephrine and a lot of these are sort of also known as happy hormones they make us feel good and these chemicals
4:41
they play a really crucial role in regulating our mood reducing stress and
4:48
enhancing those feelings of well-being yeah we also know that exercise now
4:56
stimulates the production of new neurons in the hippocampus now we all know what
5:01
to hear hippocampuses the hippocampuses and the area that is
5:07
um responsible for memory thought processing that sort of thing and when
5:12
we get deep generation on the hippocampus that's really start getting um memory loss Alzheimer's disease
5:19
dementia but we know exercise plays a big role in preventing this
5:26
so this process is known as neurogenesis and it is sort of contribute uh improved
5:34
cognitive function and reducing those neurodegenerative diseases I can
5:40
understand the same dimension um we also know that exercise and
5:46
particularly regular physical activity has been linked to improvements in cognitive abilities such as attention
5:53
memory and problem solving skills and exercise also supports the growth of new
6:00
connections between brain cells stripping those neural networks and
6:05
facilitating efficient communication within the brain so those new
6:11
connections are starting paper but the brain is actually functioning much better and of course the good old one
6:18
anxiety and stress now we know that exercise has a stress relieving effect
6:23
on the brain by reducing those stress hormones like cortisol and promotes the
6:29
release of endorphins and they are natural food boosters
6:35
so engaging in physical activity we can alleviate anxiety and depression and
6:41
enhance overall psychological well-being
6:46
improve sleep it's a regular exercise will help
6:51
regulate patterns of quality of sleep and of course will improve your sleep
6:59
and it can then also promote more or restorative sleep and
7:05
when you have got good restorative sleep we're also going to improve brain function
7:11
and then as I said before also protection against neurodegenerative diseases
7:18
um so that reduces that risk of these neurodegeneral conditions such as Alzheimer's and Parkinson's disease
7:26
and exercise may also help by protecting the brain and it reduces inflammation
7:34
okay and it promotes growth of new neurons and enhances overall brain
7:40
health so that's a in a little bit of a nutshell that is basically what regular
7:47
exercise can do to your brain but I want to stop now and I want to
7:54
focus on what's known as brain derived neurotropic Factor
8:00
because brain derived neurotropic factor that is an important protein and this
8:06
plays a role in urogenesis or the growth of new brain cells
8:12
and it's often known as the brain fertilizer right so you want to know what okay
8:18
you've got this stranger right here in public it's brain fertilizer but what
8:24
does it do okay it Spoons the creation of neurons in the hippocampus we spoke
8:30
about campus and also now exercise boosts the number of mitochondria now if you don't
8:37
know what mitochondria are they are little energy factories inside
8:43
cells and those cells are found in the brain so we get mitochondria inside ourselves and they are energy factories
8:51
they produce energy so when we exercise we actually improve the number of mitochondria so if you've got
8:59
um more of this sort of mitochondria floating around you're going to get more energy and if it's more
9:04
so in the brain the end the brain is going to have more energy so that's just going to boost brain function right
9:10
so we have these so you've got um the exercise and the increase in
9:18
mitochondria and this seems to bolster against dementia and Alzheimer's disease
9:24
so it's really the exercise the mitochondria the brain the blood flow
9:29
through the brain that's giving the brain a really good boost it's getting all these nutrients it's
9:35
also getting rid of um waste products that it doesn't want and it's getting all these little
9:41
connections happening again and it's making us
9:47
more cognitive you know where and healthy want to put it that way
9:53
so just a little uh diagram here of the brain for those of you who are not aware of brain so you
10:00
can see we've got this above campus the egg mcdela hypothalamus Thalamus and the basal ganglion so the hippocampus is
10:07
what we've been speaking about that's that little area um just next to the green board
10:14
so that hippocampus is really important for memory navigation thought processes
10:21
word processing and we often find people who have dementia and Alzheimer's
10:26
disease that little area of the hippocampus is often
10:31
um smaller it has atrophic in other words it's shrunk
10:38
right so the hippocampus is really a little important part of the brain that we need
10:44
you know to stay cognitive a way or cognitively healthy
10:50
don't you always think that one cool so if you're looking at this
10:56
bdnf or brain derived neurotropics Factor so the thing is we want to
11:01
increase the speed dnf so we can get a bit of a boost to the
11:06
brain one bit of this all this hormone it's almost like giving the brain a bit of a steroid injections when you call it
11:14
that okay but not really so if you want to increase your brain
11:20
the right neurotropic Factor the way to do this is to exercise and exercise at least 30 minutes and it
11:29
has to be daily exercise so the type of exercise that I recommend here is brisk
11:35
walking or cycling now you want to look at the experiment but how about if I tell you you can get
11:44
more bdnf if you wanted to it probably will go here I'm up for that so how do
11:50
we do this we need to increase the intensity of the exercise so a little bit more vigorous
11:57
exercise example is your identity intermittent training is really good and
12:03
a lot of research around brain and brain health and mental health is telling us that exercise is really good but we have
12:12
to increase the tempo of the exercise a little bit more to get better effects
12:18
for the brain so here we can see if you want a better increase in the ingredient in it a
12:23
little bit more I think the team post that vigorous exercise is really really good for us now you don't have to go and
12:30
do 20 000 Sprints that sort of stuff just at the tempo a little bit more like
12:35
when you're exercising you've got your moderate exercise and you've got your sort of
12:41
vigorous exercise so I would say just in between those it's a moderate and vigorous
12:47
moderately they do assignment so get the heart rate going right so between about
12:52
60 to 70 of your maximum heart rate would give a good boosting and if you can go higher
12:58
awesome the trouble now is
13:04
if we don't continue with the exercise if you stop exercising and you go back
13:10
to living on the couch right those benefits that you've built
13:16
up can what can all be wiped out by being sedentary again they even say that
13:23
if you exercise 30 minutes daily and you go back and you sit all day some of those
13:30
benefits can be lost right so if you're exercising and what
13:36
do we do a lot when we're at work we sit behind our computer screens you know all day we don't get up and do
13:43
some stuff so what they're also telling us is when are you doing some exercise you want to increase the brain function and get the
13:51
brain really working it's done sit all day every hour it should get up and just
13:58
walk a little bit and then come sit down again because you might be doing a 30-minute exercise session let's say early in the
14:04
morning you go to work and you're sitting all day some of those benefits are going to be wiped out because of
14:10
that Century behaviors all get so used to you know you work all day
14:17
finish work jump in the car go home collapse on the couch go to sleep wake up the next morning try and do a bit of
14:24
exercise and it just becomes repetitive over and over and then we wonder why we're so kind and we can't think
14:29
properly all right so let's have a look now at the best
14:35
type of exercise I reckon for a lot of people is walking and running it's the easiest type of exercise we can all walk
14:42
we can all run it just need a pair of good shoes and you could go for a walk
14:47
and now the reason why we're eating walking and running is one of the best type of exercise
14:54
because when we run and walk at an easy pace and allows the mind to wander so if
15:01
you're walking in a comfortable Pace you join in the comfortable you start thinking you know you start clearing the
15:07
mind I know if I go for a nice long walk um a bit of a job you start thinking and
15:13
you say oh you know you start thinking but clearly at times some ideas come to mind oh what
15:20
about this what about that that's that's really good because when we walk and Jog
15:26
at easy pace and the mind starts to wander this temporary temporarily
15:31
reduces activity in the prefrontal regions of the brain
15:37
okay and the prefrontal re reaches the brain they are more responsible for
15:42
rational straight line thinking and if we reduce these activities that allows
15:48
for broader more creative thinking so some companies in the states or some
15:55
companies have done a lot of work around you know exercise in the brain they'll normally go for a 15-minute walk before
16:03
they had a meeting to clear the head and to start thinking more creatively
16:10
and the the really good thing about this is when you go for a walk and you know you
16:16
start thinking more creatively these are things last for us the 15 minutes after
16:22
you've finished that activity so you know if you've got a big meeting
16:28
coming up for example uh go for a walk make sure you get back 15 minutes before
16:33
so you're not or sweaty you know then going to the meeting and you'll still have those good effects of the
16:39
exercise so a better research has also been done around uh exercise and a group of
16:48
um students for taking so they took 20 students and they looked at some of the
16:54
students that a 20-minute walk and some of the students just
17:00
set quietly before taking a test and they found after treatment of the Walk
17:05
they look at the brain and brain bunch of brain activity so that after putting my students and a lot of running
17:13
activity going on so the brains were really alive and ready to go what is those we will set quietly explain it was
17:21
decreased it's a really interesting with that one um the other thing about walking is when we
17:29
walk every time your foot hits the ground it increases blood flow back to
17:36
the brain by 13 percent right that's really really
17:43
phenomenal now some research has gone and have a look at walking in the brain and have helped
17:50
us uh how far you have to walk so they're ripping ahead 20 for 10 to 20
17:56
minutes but also they look and if you take 20 steps per minute
18:01
and your heart rate is about 120 bits per minute that is what they call a
18:07
sweet spot that just gives a rush of blood flow to the brain so if you've got a heart rate
18:14
monitor and you post yourself and you make 120 steps per minute and you've got your heart rate going at 120 beats per
18:21
minute you know you're in that sweet spot probably going to take a bit of doing to get that going but research reckons
18:28
That's The Sweet Spot to get that brain flow really going and get it going pretty well
18:36
um so the other thing that I mentioned is strength training
18:42
now strength planning is is um one of those activities that a lot of us
18:47
tend not to do as we age um but strength training is really
18:54
really important not just for the brain but for the body in general because we know as we age we all lose muscle mass
19:00
it's called sarcopena it's natural it happens to all of us so you've got to maintain muscle mass
19:06
you know to maintain functionality as we get older but researchers also now
19:13
telling us that strength training plays a really important role in brain health
19:19
and brain function in 2019 there was a study that looked at
19:26
strength and how people have declined in strengths so
19:34
in 2009 they found that this was a 30 percent
19:39
decline in muscle endurance when they compared a group of people so they
19:46
tested in 2014 and they did exactly the same case in
19:52
1998 and between that period there was a 30 decline in strict endurance but the
20:01
trouble is we are getting weaker and weaker and weaker because we're becoming more and more Centric the problem is
20:08
younger people are becoming less and less and less stronger over that becoming more weaker
20:15
so there is a problem here now you want to know well okay so what what is this going to do with the brain so when they
20:23
have a look at people who have got more strength and are more stronger they found stronger people actually do have
20:29
more gray matter okay so the brains
20:34
are a bit bigger if you want if you want to put it that way and now there's another thing here
20:40
osteocalcin Osteo calcium is a hormone that's
20:45
released from the bones when we move against gravity in any form of
20:51
weight-bearing exercise now the interesting thing about osteocalcin Studies have now linked it
20:59
to size and connectivity of the hippocampus there's the girl hippocampus again
21:06
Okay so strength training hippocampus there's a link there
21:13
and they also now have found that
21:18
our body within your body there's an unconscious sense of the health and state of our muscles and bones
21:25
so this is they call it the musculoskeletal division so your body senses
21:32
the condition of your muscles your tendons and your ligaments so what's
21:37
happening with bones now the problem here is if we're losing a lot of strings
21:45
these messages that are consistently being sent around the body
21:51
uh our strength our agility and our movement apparatus so if these messages
21:58
are going around and are telling us well hang on this is not looking too good this is
22:04
going to have effect on your sense of well-being and feeds into the implicit sense of what we
22:11
can handle okay so the body knows well I can handle this I can't handle that there's an
22:17
underlying sense in our bodies and the problem here is we
22:23
see decreasing levels of strength in modern society
22:28
and this might play a part of an increasing levels of anxiety and depression that we are seeing a lot of
22:34
now a good example of strength and brain and anxiety and depression
22:43
strength training and physical strength is often seen uh it's
22:50
not often seen as linked to self-esteem so you a lot of people are physically
22:55
strong and healthy seem to be you know they've got a lot of self-esteem they feel good they feel
23:01
healthy they feel empowered now a really good example here is um two or three years ago we did a study
23:08
in Linton where we looked at our females and strength training because a lot of
23:13
our females were um having trouble with the land combat fitness test particularly the upper body
23:20
components the strength components because we all know the differences between males and females is upper body
23:27
stream so we did a strength training program put our females uh
23:34
on the the study and it was an intervention 20 it was 12 weeks
23:39
currently remember but after the exercise with the strength training program they had no problems in passing
23:47
the land combat fitness test their regular Fitness label case they smoked
23:52
them they actually came to us and said we smoke these and the the best thing about that when we spoke
24:00
to these females post the exercise poster training a lot of them said to us I've never felt so empowered
24:07
in all my life after I've done this training program and I kid you not some of these
24:14
um ladies were lifting weights that I can barely get off the ground and the look The problem is with a lot
24:21
of females and strength training a lot of females think that if I do strength training I'm going to get big muscles
24:26
that's not the case that big muscles has got a lot to do with hormones testosterone estrogen so
24:34
ladies you won't keep with muscles if you do a lot of strength between there's a neurological effect
24:40
right so strength training is pretty important and it's really important to
24:45
get that sense of well-being to be strong and healthy and it does have a really good positive effect on the brain
24:52
I know a lot of people who do a lot of strength training after strength training you feel really good about yourself because you've accomplished
24:59
something now the thing is we're strength training you don't have to go to the gym and push
25:06
heavy whites there's a lot of other stuff we can do you know you can't do resistor training
25:11
you can do weights there's nothing wrong with doing weights weights are really good for us
25:17
body weight exercises just use your own body weight set up squish UPS all that kind of stuff and rubber bands rubber
25:23
bands is another great way to do exercise there's various ways of increasing your strength and exercise
25:33
and you really have those good benefits so if we have a look at
25:39
but it's like here exercise their Mental Health exercise really does have good positive
25:45
effects on mental health so you can see there you know those happy chemicals that I spoke about earlier it really
25:51
does get those going self-confidence especially those who increase their strength levels strength training uh
26:01
Outdoors if you go for your walk you know you get a nice boost of vitamin D which is really
26:07
important across as well that cognitive decline within their anxiety
26:14
it's a good way to relieve the anxiety and we do know now that we are seeing a
26:19
lot of anxiety and depression in our organization because of the high workloads of that number of people that
26:26
are leaving and interestingly again we looked at an over 40s program we ran in
26:32
Linton um it was just after the first covert we all came out
26:38
of lockdown we did a program we did some measures on anxiety and depression at
26:44
the start of the program we had very high levels of anxiety and and much of
26:49
bad on the depression scale but they were quite up there um good at exercise intervention for
26:55
people particularly in that age group of over 40 post exercise those levels
27:01
dropped significantly just after doing some good exercise and
27:07
targeting at that level a lot of us don't go to exercise or don't go to the
27:13
gym because it's too many young people I know a lot of people who are older
27:19
should say a little bit more senior you know one exercise programs that are more tailored for them so for us
27:26
um and that's good at the moment but just remember you know when you exercise don't forget your strength training
27:32
don't forget Joy Rogan as that all are really important for us um brain power memory relaxation really
27:40
good for relaxation the thing is with exercise and
27:45
relaxation you can do different type of exercises to help you relax yoga is a really good one dancing
27:52
dancing is really really good for the brain because when you dance you've got to think you know there's the
27:59
choreography you've got to think of the steps you're taking so you've got to think while you're exercising another
28:04
good um way to exercise and get the brain going is often you'll go to the gym and
28:10
on the treadmill they'll have card games solitaires one that I've seen so while you're doing your walk on the treadle
28:17
play some Solitaire that gets the brain going while you're doing exercise
28:22
what um that just helps us be more productive and also I've said before it also
28:29
reduces stress so there are many many benefits of doing some exercise
28:34
all right to help the brain not just the body healthy mind healthy body we all
28:40
know that but it's good to know that you know exercise does really help
28:46
our brains and the more we exercise the better it is for us
28:52
and then there's the whole thing you know get into a habit if so should become a habit but that's a whole
28:57
different talk yeah it's an exercise are there
29:04
any questions uh for anyone listening at home feel free to check in your questions on the
29:09
chat now we can uh ask them in person here
29:17
do you think it's better to exercise in the morning when you get up to start your day and get everything Reef up or
29:23
later um you know early evening or is that going to rub your brain have too much to
29:29
sleep no no no that's a really good that's a really good question and that question comes up quite regularly
29:36
um particularly when it comes to cognitive function the brain and exercise um
29:42
a couple of years ago in the U.S they did a big study on exercise and physical
29:48
conditioning or physical education and they went into the schools and they got a lot of the kids to do PE
29:56
before they started school and they took the subjects they look at with science
30:01
and maths um they put them straight after the PE classes and the PE classes were
30:09
developed so each child had to reach a certain heart rate they weren't given their own heart rate monitors and it was
30:15
about it was getting them up to that little sort of the biggest level of exercise so it was self-led and a lot of
30:23
the children brought into the exercise program and they found that after the
30:29
the training when they went into their maths and their science the grades
30:35
skyrocketed so that early morning exercise going to the exercise before you've got to go and
30:41
do some you know thinking or subjects where you've got to think a lot really did improve so it depends what you're
30:48
doing I mean you can exercise in the morning you can exercise it doesn't really matter but if you want to get that real push of
30:57
Brian and get that cognitive function going they're reckon exercise in the morning sets you up for the day
31:03
because it gets that blood flow going to the brain and gets the all those little connections going
31:09
um and it makes you think clearer clearer yeah so yeah so in the morning
31:16
I would reckon if you've got you know sitting himself for the day a good morning session would be really good
31:21
um lunch time if you've got meetings coming up in the afternoon go for a nice walk perhaps and then
31:28
and get back to the office but they do reckon a lot of exercise around exercise in the brain it doesn't
31:34
cognitive function does talk about that morning exercise yeah
31:42
but then there was a good program I think it was last night about sleep and exercise do
31:48
we need more sleep or do we need to exercise more we need both because sleep as we're getting tomorrow
31:53
is really really important for us as well and that's also important for the brain
31:59
so you need good quality sleep but you also need good exercise so don't
32:04
compromise your sleep you know just because you really have to wake up at four o'clock in the morning exercise
32:10
session do your exercise later on in the day now as long as you're doing some form of
32:16
exercise we've just got a question in the chat from the people at home from Richard and
32:22
they say how does VO2 max fit into your brain health well VO2 max obviously
32:28
virtual Max is your maximum oxygen advocate so the more oxygen your body
32:33
can utilize and use the better it is going to be for your brain so if we increase VO2 max we're going to
32:40
increase oxygen uptake and of course you know the body and the Brain the circulatory system work together so you
32:48
will then increase the oxygen uptake to the brain as well so that blood flow
32:54
will go more so we'll be more oxygen going to the brain and more nutrients as well that would definitely
33:01
help with brain function and common to function yeah because it's not just a lung thing it's
33:07
a frying thing as well yeah I've also got another question that asks uh when is the latest time you should be
33:13
exercising before going to sleep so especially if you have a higher heart rate that's a good one so if you
33:19
um and we've talked about this a lot more in tomorrow's talk about sleep so they really can you should not exercise
33:25
on your last exercise should be an hour before you go to bed
33:31
but ideally three hours before you go to sleep because when we exercise the core temperature increases and then that can
33:38
stop you from getting to sleep but you don't want to go to bed when the body is too hot
33:44
right so you want to get experience when you've cooled down a little bit and you've relaxed a lot more so exercise
33:50
before sleep is really good but try and limit that to about three hours before there's a lot of research in that area
33:56
as well saying that exercise before sleep is actually okay but it depends on the type of exercise if you're doing
34:03
meditation yoga that sort of exercise or activity that might help better but if
34:09
you're going to do sort of vigorous exercise where you're going to run you know and get the heart rate up to about 70 80 percent of Max now let's just keep
34:17
you awake for a lot longer
34:25
together questions unspoken
34:37
and so the questions so far online if anyone else has any more listening at home Chuck them through now
34:43
foreign
35:00
there will be a recording of This seminar there will be released so you can come back and watch it again if
35:05
there's anything you missed if there's anything you want to re-go over cool thanks for coming in I'll be finishing
35:11
up now okay